Stuart Richardson was appointed as Chief Operating Officer of Norfolk and Suffolk NHS Foundation Trust (NSFT) under the leadership of former Chief Executive, Antek Lejk and former Chair, Gary Page and started his job on 1st August 2018. One year ago today. Managing beds is his responsibility.
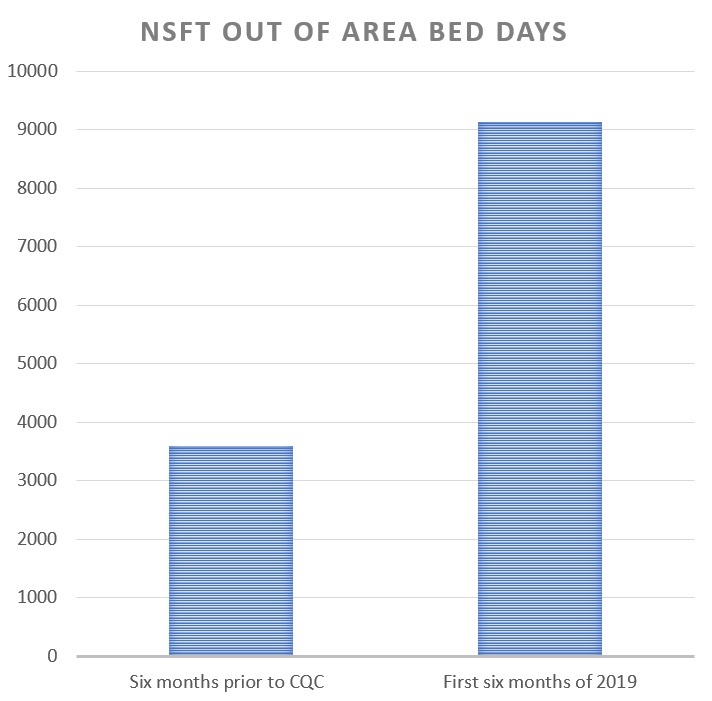
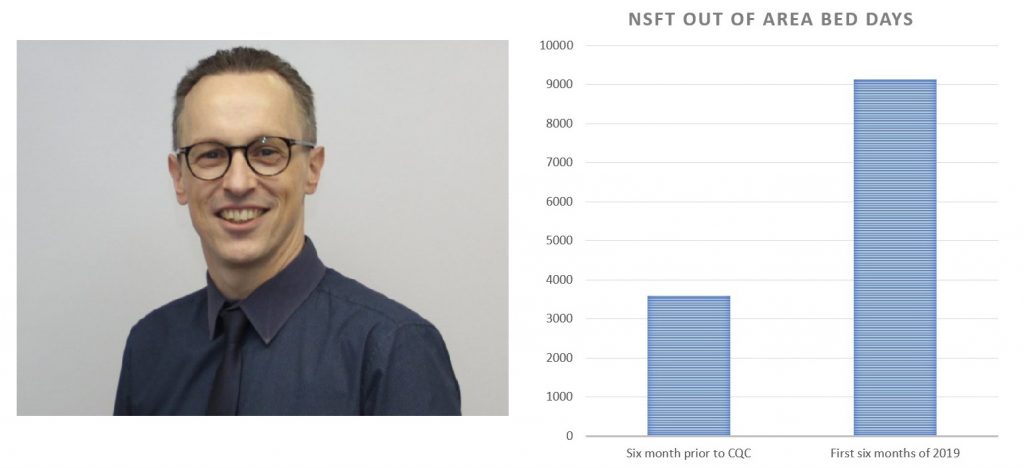
In the six months immediately before Stuart Richardson joined NSFT, between February and July 2018, NSFT transported people in crisis for a total of 3,595 bed days. In addition to the human misery, at an average cost of £550 per bed per night, this will have cost the NHS about £1,977,250.
For the latest six months available, between January and June 2019, Stuart Richardson managed to set new records, even by the dire standards of NSFT. NSFT transported people in crisis for a total of 9,131 bed days. In addition to the human misery, at an average cost of £550 per bed per night, this will have cost the NHS about £5,022,050.
So, in return for Stuart Richardson’s six-figure annual salary, the people of Norfolk and Suffolk have seen the already intolerable number of out of area bed days more than double and been landed with additional costs of more than £3 million. Over just six months. From where will this money come?
In the month before the latest CQC inspection failure, August 2018, the same month that Stuart Richardson started at NSFT, there were 565 out of area bed days. The latest month available, June 2019, shows 1,385 out of area bed days, which is a 143 per cent increase on August 2018. April 2019, when Stuart Richardson had been in post for eight months, saw a staggering 1,911 out of area beds days, more than three times the number when Stuart Richardson started in August 2018 and the highest ever recorded at NSFT.
In each of the first six months of 2019, the number of out of area bed days at NSFT has been higher than at any time since NHS Digital started recording the information in April 2016, more than three years ago.
Let’s put this in perspective: in the year before the cuts and chaos of the radical redesign, 2012-13, NSFT sent six (6) patients out of area. During the entire year.
What do we think caused this massive deterioration in operational performance?
It wasn’t just chance.
We warned both the new trust chair, Marie Gabriel, and the new Chief Executive, Jonathan Warren, about what was going on in their first days in their jobs.
We believe Stuart Richardson thought he would ‘sort out’ bed management and the crisis and home treatment teams and secure his position in NSFT’s internal politics: people were pushed out with wasteful and massive settlements; henchmen were sent in; front line staff were marginalised, ignored and demoralised; services were clumsily rearranged; front line clinicians tell us they were bullied and many went off sick, retired or got jobs elsewhere. The result was operational chaos.
While front line mental health services were going into meltdown, Stuart Richardson was preoccupied with the disastrous and shambolic ‘radical restructure’ which had virtually no input from front line clinicians and was not co-produced.
Those around Richardson, some the same people responsible for the meltdown in crisis services, secured senior positions in the new structure. Worse still, not seemingly knowing or caring about what had happened before, many of those re-employed or promoted were deeply involved in the ‘radical redesign’ and the failures of the past six years.
Let’s be frank about this: people died as a result of the radical redesign; some campaigners buried their children.
We told Marie Gabriel and Jonathan Warren face-to-face that they should stop or delay the ‘radical restructure’ but they ignored our advice. Now we can see the results of that fatal mistake.
While NSFT claimed it was reducing its layers of bureaucracy, Richardson appointed himself a deputy and a scandalous appointment at that.
Meanwhile, in contrast, there has been no lead clinician in mental health services in Norwich, the area in the greatest chaos, for months. The newly-appointed Clinical Director, deeply implicated in the disaster of the radical redesign, does not start until September but the previous Lead Clinician gave up their role months ago. The right candidate wouldn’t have tolerated a vacuum in clinical leadership and would have got to work straight away.
These are the priorities and values of ‘clinically-led’ NSFT. We can’t imagine what the CQC will think when it inspects in September. How can a ‘clinically-led’ NHS trust leave large areas without clinical leadership for months or allow the number of out of area bed days to go through the roof?
The ‘radical restructure’ shambles should have been stopped before it started and Stuart Richardson should have been sacked months ago. Every day he remains Chief Operating Officer is a day wasted and an insult to the hundreds of additional people transported across the country.
This is a scandal. People with serious mental health conditions need prompt service when they are in crisis, locally and in places of safety. Whilst managers run back and forth attending futile meetings around Norfolk and Suffolk, rewriting strategies and restructuring already inadequate services, people are suffering and some are dying. The mental health service has degenerated into an unresponsive, poorly managed crisis service. Frontline staff continue to struggle on trying to deliver a genuine service to improve the lives of vulnerable people and keep them safe, but directors sit in meetings strategising. If they think their inadequacies will be submerged in the promised delivery of integrated care systems promised by April 2021 by the Sustainable Transformational crew, they should think again.
When Richardson goes, he needs to take Amy Toxic Eagle with him! She can’t ever be forgiven in this life.
This article opened my eyes, I can feel your mood, your thoughts, it seems very wonderful. I hope to see more articles like this. thanks for sharing.
Thanks for sharing. I read many of your blog posts, cool, your blog is very good. https://accounts.binance.com/bg/register?ref=IQY5TET4
Its not my first time to pay a visit this web page, i am browsing this website dailly and obtain good
data from here all the time.
Take a look at my blog … vpn coupon code 2024
WOW just what I was looking for. Came here by searching for vpn special
What a data of un-ambiguity and preserveness
of precious familiarity on the topic of unexpected feelings.
Here is my web-site :: vpn special coupon code 2024
Does your site have a contact page? I’m having trouble locating
it but, I’d like to send you an email. I’ve got some ideas for your blog you might be
interested in hearing. Either way, great site and I look forward
to seeing it develop over time.
Also visit my site; vpn coupon 2024