‘S’ writes:
“One of my neighbours lives in South Norfolk, in the Diss area. He has been under under-65 services for many years as he has suffered from the enduring mental health issue of depression. This ebbs and flows; this year he is very low in mood, he was discharged from the service because they felt he was not engaging well enough with the service – he is depressed and struggles to get motivated! Within 2 weeks he was struggling even more. A Crisis referral was made to the services – two months later he was asked to attend the Norfolk & Norwich University Hospital in Norwich – No CMHN allocated, NO medication changes, his wife feels completely at a loss about what to do.
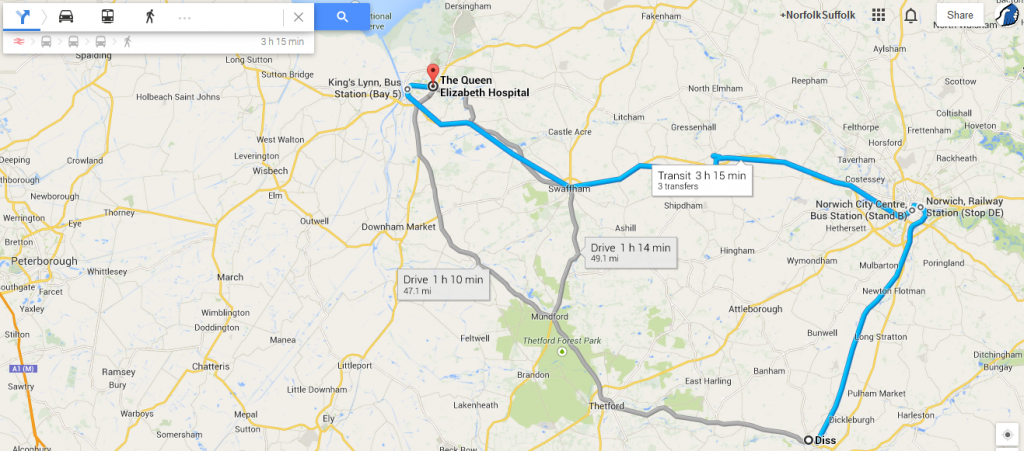
Yesterday 3 months after his GP referral he has been offered a ‘chat’ with a member of the adult team in KING’S LYNN … remember he lives in DISS.
Not sure If I can understand the reasoning on this, or am I missing something? So the moral of the tale is:
- Boot off unwell people as they don’t comply, they’re too ill
- Don’t accept a referral in the first place
- Make a new response target of 2 months.
- Make an appointment 3 months after a GP referral and make it at the northernmost place in the county you live in!
- Maybe the patient won’t make the appointment to come to the hospital as they are so ill they might fail to turnn up; so close referral, send GP a patient did not attend letter.
Or am I still being cynical? And yes, I did not make this story up, I know this man, he is my neighbour. And the letter asking him to attend King’s Lynn does exist…”