A Campaign spokesperson said:
“The decision of the Board of NSFT to remove the number of unexpected deaths from its Annual Report and Accounts 2015-16 is disgraceful. The number of NSFT patients dying unexpectedly increased by thirteen per cent in 2015-16 and continues to do so. Since April 2012, at least 572 NSFT patients have died unexpectedly; the number has increased every year. Based upon the first five months of 2016-17, more than 200 NSFT patients will die unexpected deaths this year, which will take the total since April 2012 above 750. NSFT claims to take the deaths of those who rely on its services seriously but then removes their number from the trust’s document of historical record. This is shameful.”
At the AGM, NSFT will publish its Annual Report and Accounts 2015-16.
This is our guide. Page numbers refer to the NSFT Annual Report and Accounts 2015-16.
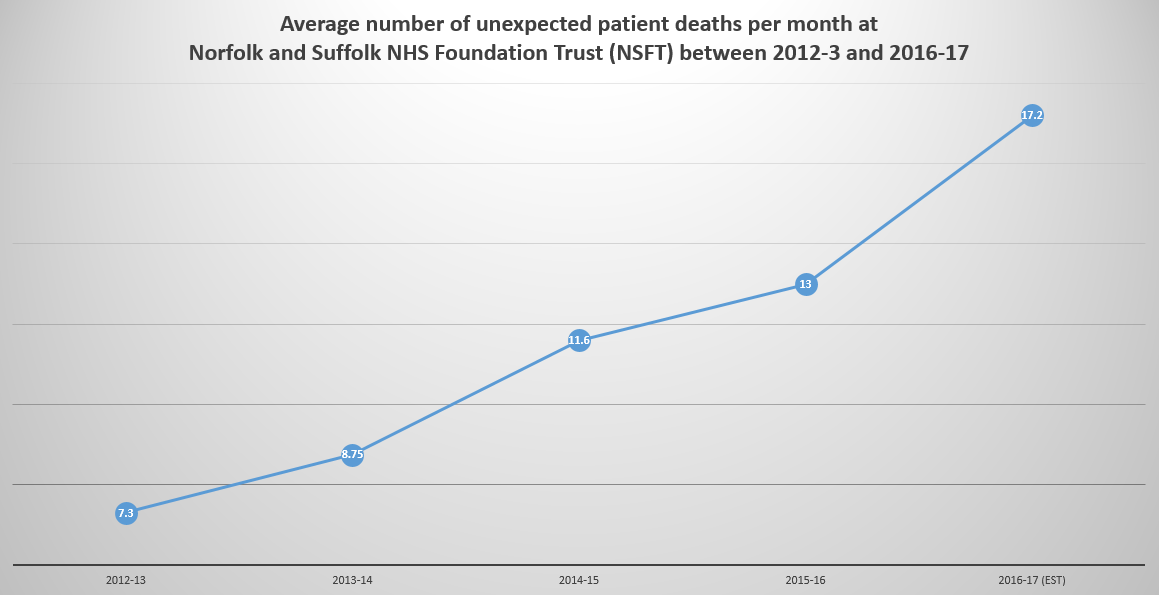
At least 572 ‘unexpected deaths’ since April 2012 and still rising
- Norfolk and Suffolk NHS Foundation Trust (NSFT) has removed the number of unexpected deaths from the Annual Report 2015-16 (previously these would have appeared at page 110)
- Every Annual Report produced by NSFT since its foundation until this report has contained the number of unexpected deaths (see images below from all published full-year reports)
- If NSFT had not deleted the number of unexpected deaths from the Annual Report 2015-16, it would have reported 157 unexpected deaths (13 per cent annual increase)
- The Care Quality Care (CQC) Inspection Report of October 2016 rated NSFT ‘Inadequate’ for Safety and stated ‘we are concerned that overall rates of death remain high at the trust’
- The NSFT Annual Report and Accounts 2015-16 is 176 pages in length and contains 70,717 words
- The number of unexpected deaths has increased for the last four consecutive years
- The number of unexpected deaths was reported in the Annual Report 2012-13 as 53 but was later restated in the press as 88 (NSFT has never produced the basis of restatement)
- The Campaign uses the unexplained restatement as the basis of conservative calculations
- The number of unexpected deaths reported in the Annual Report 2013-14 was 105
- The number of unexpected deaths reported in the Annual report 2014-15 was 139
- There was a 78 per cent increase in unexpected deaths between 2012-13 and 2015-16
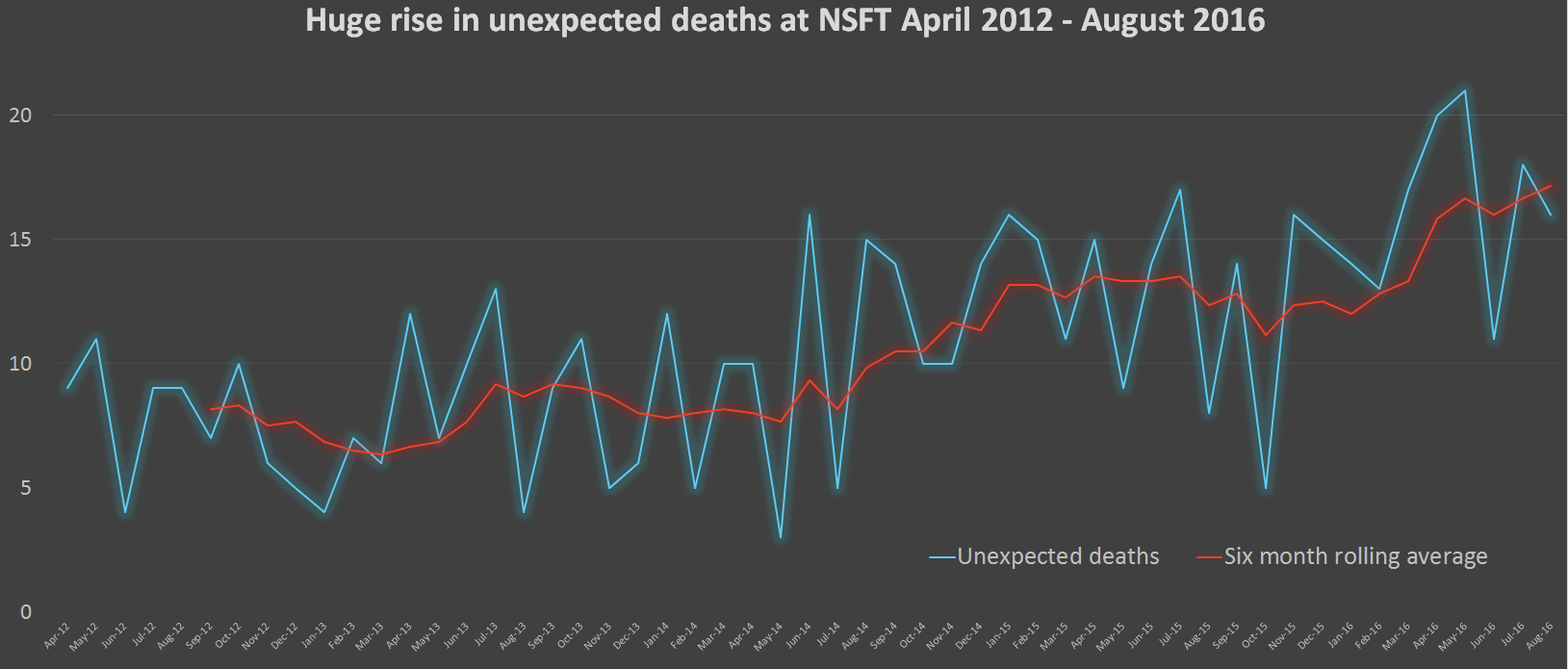
- The number of unexpected deaths continues to climb
- In the first five months of 2016-17, there were 86 unexpected deaths (nearly as many as in the whole year of 2012-13)
- If the number of unexpected deaths continues at the rate of the first five months of 2016-17, there will be more than 200 unexpected deaths this year (206), representing a 134 per cent increase in just four years (2012-13)
- NSFT’s Five Safety Priorities did not include reducing the number of unexpected deaths (page 106)
53 (88) unexpected deaths in 2012-2013
105 unexpected deaths in 2013-14
139 unexpected deaths in 2014-15
Number of unexpected deaths removed in 2015-16
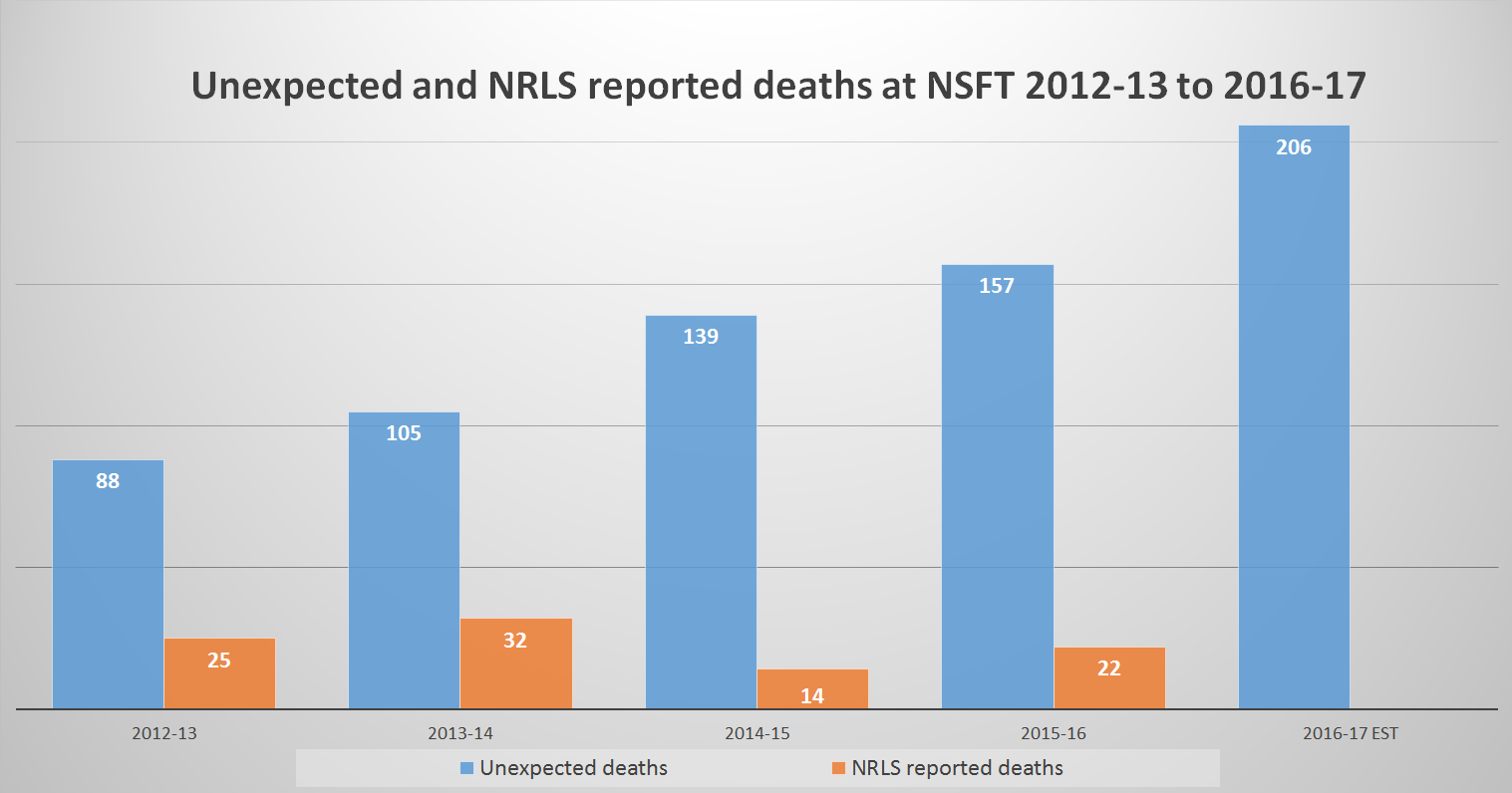
Incident reporting data (NRLS) deaths reduce as unexpected deaths increase?
- Since NSFT’s removal of the number of unexpected deaths from its Annual Report 2015-16, the only statistics on patient deaths present are those reported in QA12 Incident Reporting
- One of NSFT’s Five Safety priorities is ‘To ensure NSFT embeds a safety culture based on openness, transparency and learning from previous incidents that have caused harm’ (page 106)
- At the Health Overview and Scrutiny Committee of Norfolk County Council, the Chief Executive and Patient Safety Manager of NSFT told councillors that its methods of methods of recording and reporting of patient deaths have remained unchanged since 2012
- Has NSFT unilaterally changed its interpretation of the National Reporting and Learning System (NRLS) to reduce the number of deaths reported?
- In 2012-13, 25 deaths were reported to NRLS from 88 unexpected deaths (28 per cent)
- In 2013-14, 32 deaths were reported to NRLS from 105 unexpected deaths (30 per cent)
- From 2014-15 onwards, the proportion of unexpected deaths reported to NRLS suddenly drops by up to two-thirds
- This drop coincides with the foundation of our Campaign and staff and public concern over the increasing number of patient deaths
- In 2014-15, only 14 deaths were reported to NRLS from 139 unexpected deaths (10 per cent)
- In 2015-16, only 22 deaths were reported to NRLS from 157 unexpected deaths (14 per cent)
- However, if NSFT had reported on its former basis, the number of deaths reported in 2014-15 would have been 34; the number reported in 2015-16 would have been 53 (this calculation takes the average reporting percentage before the change as 29 per cent and 12 per cent thereafter)
- Without the suspected ‘drop’ in reporting, the number of NRLS deaths would have increased from 25 to 53 (112 per cent increase) in only three years, an annual rate of increase of more than 37 per cent
- With the suspected ‘change’ in reporting, the number of NRLS deaths appears to have decreased from 25 to 22 (12 per cent decrease) in the three years, an annual rate of decrease of about four per cent
- This calculation is conservative because one would expect the proportion reported to rise as the number of natural causes remains broadly stable in a fixed population in the absence of war or epidemics
- The Campaign to Save Mental Health Services in Norfolk and Suffolk has sought a response to our specific questions about NRLS reporting from NSFT but has not received a satisfactory response to our questions other than a link to the NRLS website (can supply to media on request)
- The Campaign to Save Mental Health Services in Norfolk and Suffolk has reported its concerns about NRLS reporting by NSFT to both its regulators: the Care Quality Commission and NHS Improvement
What is an unexpected death? Anatomy of a catastrophe
- In the four months February, March, April and May 2016 there were 94 Serious Incidents (SIs)
- Of these SIs, 71 unexpected deaths of NSFT patients were reported in the four-month period
- Average of 18 unexpected deaths per month
- 66 (93 per cent) of the unexpected deaths were community patients
- 29 (41 per cent) of the unexpected deaths happened to patients under NSFT community mental health teams
- Of these 29 unexpected deaths, 18 (62 per cent) were the deaths of patients under the Central Norfolk community teams
- 17 (24 per cent) of the unexpected deaths were patients of the drug and alcohol service, NRP
- 7 (10 per cent) of the unexpected deaths were patients of the Norfolk Wellbeing Service
- 3 of these patients had either been discharged from the Wellbeing Service or were waiting to be seen
- 4 (6 per cent) of the unexpected deaths were patients of Psychiatric Liaison Services
- 3 (4 per cent) of the unexpected deaths were patients of AAT/AFI
- 2 (3 per cent) of the unexpected deaths were patients of the crisis team (CRHT)
- 29 (41 per cent) of the unexpected deaths happened to patients under NSFT community mental health teams
- 5 (7 per cent) of the unexpected deaths were inpatients
- 2 (3 per cent) of the unexpected deaths happened on older people’s wards
- 2 (3 per cent) of the unexpected deaths were choking deaths on adult acute wards
Performance
- The number of patients waiting more than eighteen weeks for treatment rose from 78 in 2014-15 to 280 in 2015-16. This is an increase of 259 per cent (page 103). Delayed access to treatment increases suicide risk
- The proportion of patients having access to the crisis team prior to admission fell from 98.2 per cent in 2014-15 to just 60.62 per cent in 2015-16. This is a decrease of 38.2 per cent and is 36 per cent below target (page 103). Difficulty accessing crisis services increases suicide risk
- The proportion of patients having follow-up with seven days of discharge fell from 98.57 per cent in 2014-15 to 89.42 per cent in 2015-16. This is a decrease of 9.3 per cent and is 5.8 per cent below target (page 103). Suicide risk is increased in the absence of follow-up within seven days
- The number of CPA patients having an annual review has fallen from 96.71 per cent to 69.24 per cent. This is a decrease of 28.4 per cent and 27 per cent below target (page 103). CPA review is an indicator of high-quality services
- There were five admissions of children to adult wards (page 103). Children should never be admitted to adult wards
- The proportion of patients readmitted to a hospital which forms part of NSFT within 28 days of being discharged from a hospital which forms part of NSFT has increased from 5.3 per cent in 2013-14 to 8.33 per cent in 2015-16. This is an increase of 57 per cent in the last two years, indicating that people are being discharged before they are ready and that there are insufficient beds (page 97). It is very bad for the patient and expensive for the NHS. It appears that these statistics do not include patients placed in private hospitals or in other NHS Trusts, so it is likely that readmission rates including these would be worse still
- The ‘patient experience’ of community mental health services has declined from 8.6 in 2013-14 to 7.3 in 2015-16, a fall of 15 per cent (page 100)
Staffing
- The CQC Inspection Report of October 2016 states ‘We were concerned that staffing levels, including medical staff, were not sufficient at a number of inpatient wards and community teams across the trust’
- Average staff pay has fell by 4.4 per cent, from £28,180 to £26,947 (page 32)
- The number of doctors employed by NSFT in 2015-16 was 160 (page 47). In 2012-13, NSFT employed 268 doctors. This represents a cut of more than 40 per cent in the number of doctors
- The number of nursing staff employed by NSFT in 2015-16 was 1132 (page 47). In 2012-13, NSFT employed 1250 nursing staff. This represents a cut of nearly ten per cent in the number of nursing staff
Finance
- NSFT’s operating income has fallen by £7.6m since 2012-13. This is a fall of £7.6m (3.5 per cent) in absolute terms but a fall in real terms of 13.2 per cent (2012/3 RPI = 3.6%, 2013/4 RPI = 3.3%, 2014/5 RPI = 2.5%)
- NSFT’s total operating income fell from £212.8m in 2014-15 to £211.8m in 2015-16. This is a fall of 0.5 per cent in absolute terms but a cut of three per cent in real terms (page 138)
- NSFT’s total operating income in 2013-4 was £216.8m
- NSFT’s total operating income in 2012-13 was £219.4m
- NSFT’s operating deficit doubled from £2.02m in 2014-15 to £4.07m in 2015-16 (page 138)
- NSFT’s deficit was £8.91m in 2015/6 (page 138)
Executive Pay
- The Fair Pay ratio has worsened by 3 per cent from 6.3 to 6.5 (page 32)
- Chief Executive Michael Scott’s total remuneration including pension benefits was between £360,000 to £365,000 per year (page 28). Michael Scott’s salary is higher than that of the Prime Minister (page 23)
- The salary paid to the Director of Finance at NSFT was increased by £5,000 from £125,000 to £130,000 p.a. (page 22)
- NSFT Finance Director Julie Cave left Norfolk and Norwich University Trust on 13 September 2015 (see NNUH Annual Report page 74). She joined NSFT on 1 December 2015
- The former NSFT Director of Finance, Andrew Hopkins, left NSFT on 13 September 2015 and joined Norfolk Community Health and Care NHS Trust on 1 March 2016 (see NCHC Annual Report page 60)
- Andrew Hopkins and Julie Cave appear to have had periods of not working for the NHS for approximately six and three months respectively when moving between NHS organisations yet appear to have been ‘compensated’ throughout
- It appears that while the Director of Operation for Norfolk and Waveney (Kathy Chapman) was on ‘secondment’, she was paid as an Executive Director in 2015-16 but NSFT does not report her remuneration in the Accounts (page 59)
- NSFT’s 2014-15 Annual Report stated that Dr. Chapman was on ‘Secondment with NHS England’ (page 100)
- NHS England told the Campaign to Save Mental Health Services in Norfolk and Suffolk in a Freedom of Information Act response that Dr. Chapman did not work for NHS England
Best Practice / Evidence-based Approach
- The University of Manchester hosts the Centre for Suicide Prevention publishes the National Confidential Inquiry into Suicide and Homicide by People with Mental Illness
- The most recent report was published on 6th October 2016
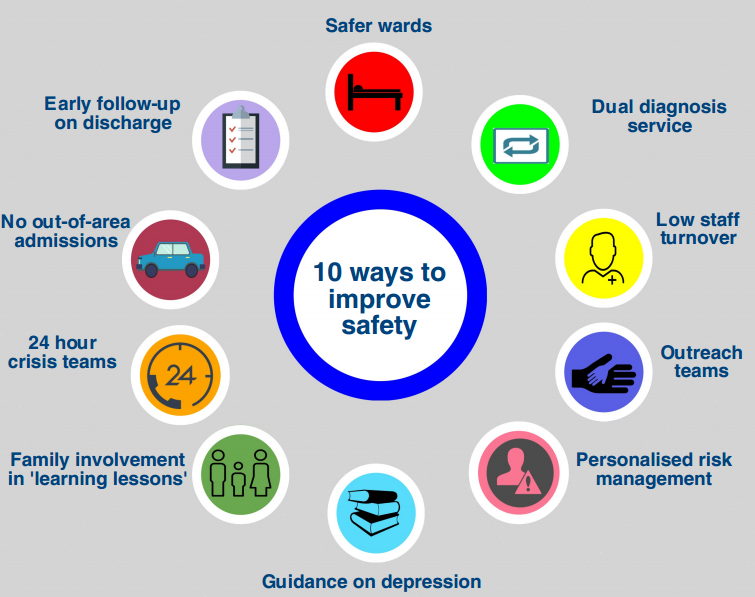
- It has published an infographic ’10 Ways to Improve Safety’, reproduced below
Considering each recommendation in turn:
- Safer wards
- NSFT has again been criticised by the CQC for the safety of its wards with the CQC reporting ‘We found a number of environmental safety concerns. Whilst some work was being planned or underway to remove potential ligature risks, we were concerned that planned actions would not adequately address all issues. We also found that the layout of some wards did not facilitate the necessary observation of patients’
- Should inpatients be choking to death on NSFT wards? The CQC reported in October 2016 ‘Of particular concern were levels of training in restrictive intervention and life support’
- Early follow-up on discharge
- NSFT missed its 7-day follow-up target in 2015-16
- Performance deteriorated by 9.3 per cent since 2014-15
- No out-of-area admissions
- The last two CQC Inspection reports have stated that NSFT has insufficient beds
- In its report of October 2016, the CQC said ‘A lack of availability of beds meant that people did not always receive the right care at the right time and sometimes people had been moved, discharged early or managed within an inappropriate service’
- Last month, NSFT had more than thirty patients in the private Mundesley Hospital alone and has ‘blown’ its out of area/trust budget
- In September 2015, NSFT closed Waveney Acute Services at Carlton Court near Lowestoft with the loss of at least 10 inpatient beds
- In Spring 2016 NSFT attempted to close the Fermoy Unit at King’s Lynn which would have lost 20 acute adult beds. Five beds have been closed at the Fermoy Unit reducing the number of beds to 15
- Despite two CQC reports stating that NSFT does not have enough beds, rather than stopping ward closures and opening more beds, NSFT is instead spending £75,000 with management consultants to find out whether it has enough beds or not
- 24 hour crisis teams
- The proportion of patients having access to the crisis team prior to admission fell from 98.2 per cent in 2014-15 to just 60.62 per cent in 2015-16 (page 103)
- Crisis teams have lost experienced staff and have less medical input
- Crisis support for children and young people is deeply inadequate in Suffolk
- Outreach teams
- NSFT has closed its Assertive Outreach and Homeless teams contrary to need and evidence
- Dual diagnosis service
- NRP’s electronic record system is incompatible with NSFT’s mental health systems
- 20 per cent cuts to NRP have already seen its medical component fall considerably
- Further cuts of another 20 per cent to NRP threaten to virtually eliminate its medical and nursing staff and increase the burden on already overstretched community teams
- Family involvement in ‘learning lessons’
- NSFT is poor, even referring to the wrong patient in condolence letters from the Chief Executive
- We introduced unhappy families to the CQC during their recent visit
- The CQC stated in its October 2016 Inspection Report ‘The trust had systems in place to report incidents however we found a number of incidents across the trust that had not resulted in learning or action’
- Guidance on depression
- There seems to be a dangerous gap in provision for high risk patients between the Wellbeing Service and acute adult psychiatry at NSFT
- Personalised risk management
- In its October 2016 Inspection Report the CQC stated ‘The trust had not ensured that all risk assessments were in place, updated consistently in line with changes to patients’ needs or risks, or reflected patient’s views on their care’
- Low staff turnover
- NSFT does not have enough staff with the CQC stating ‘We were concerned that staffing levels, including medical staff, were not sufficient at a number of inpatient wards and community teams across the trust’
- NSFT has high staff turnover
- NSFT wasted £20m paying its most experienced and highly-trained staff to leave the trust’s employment
- NSFT employs a high number of agency staff
You can download this guide as a pdf document.





And the unexpected deaths do not take into all those poor frail older people moved hundreds of miles for a bed because the trust didn’t have any, and then died out of area. Where’s the stats on those, because I can guarantee that their frail, confused, poor physical states were NOT improved by carting them all over the country often hundreds of miles to find a bed.
?????, ??? ?????????? ?????? ? ??????? ??? ?????? ????????????? ???????? ?????????? ?????? ????????? ??????? ????????? ? ????????? ?? ???? ??????.
??????? ??????? ? ?????? – ??? ??? ???????????????? ????????, ????? ?????????? ?????? ???????? – https://diplomsuper.net. ? ?????? ??????????????? ????? ????????? ??? ?????? ?????????????.
? ??????????? ??????????????? ?????? ??????? ????????????? ??????? ???????????? ??? ??????? ?????? ??????????? – diplomex.com. ??? ?????????????? ??????????? ?????????? ?? ??????? ? ?????????? ??????? ????? ? ???????? ????????? ??????????? ??????????. ?????????? ????? ?????, ????? ? ???????????? ????????, ????????? ?? ??? ???????????, ?? ???? ?????? ?????????. ?????? ??????????? ???????? ????? ??????????, ???? ?????????? ?????? ? ?????????? ???????????, ????????? ???????? ????? ????????? ? ????????? ?? ????? ????????. ??????????? ?????? ??????? ? ?????? ?????? ??????????? ???? ???????? ????? ?????? ??????????????? ???????? ???????, ??-?? ????, ??? ??? ?? ??????? ????????? ????? ?? ?????-???? ????????, ????? ???????? ????????? ??????????????? ?????. ??????, ???? ??? ???????? ?????????? ??? ?????????? ?? ??????, ? ???????? ????? ??????? ????? ????????.
? ??????? ?????? ???????? ?????? – ??? ?????????? ? ???????? ?????? ????????? ?????? ?????? ???????? ?????????????? ??????????. ????????? ???????? ?????????? ?????? ?? ???????????? ? ?????????? ???????? ?????? ??????????????? ?????????? – [URL=https://diplomkupit.org/]www.diplomkupit.org[/URL]. ??????????? ???????????? ? ?????? ?????, ??????? ????????? ? ????????????? ? ??????? ???????????, ?????????, ??????? ????? ? ?????. ??????? ???????????? – ??????????? ??????? ?????? ???????, ?????????????? ??????????? ? ??????? ????????. ??? ????????????? ??????????? ?????? ??? ???????? ? ????????????? ??????????? ????????? ???????? ??? ????????????? ?????. ????? ?????, ????? ????????????? ? ?????? ?????? ???????? ?????? ?????????? ? ??????????? ??????? ??? ?????, ??? ????? ??????? ?????? ? ????? ??????.
? ??????? ?????? ???????? ???????? – ??? ??????? ? ??????? ????? ????????? ?????? ?????? ???????? ?????????????? ??????????. ??????? ?????????? ???? ??????? ?????? ?? ???????????? ? ?????????? ???????????? ?????? ??????????????? ?????????? – diplom4you.net. ??????????? ???????????? ? ?????? ???????, ??????? ???????????? ? ?????? ?????? ? ?????????? ???????????????? ??????????, ?????????, ????????????? ????? ? ????????. ???????? ??????????? – ??????????? ??????? ?????? ??????????? ????????, ????????????? ?????????? ? ??????? ????????. ??? ??????????? ??????????? ?????? ??? ???????? ? ????????????? ??????????? ???????????? ????????????? ??? ????????? ?????. ????? ????????, ???????????? ??????? ? ?????? ?????? ???????? ???????? ? ??????????? ??????? ??? ???, ??? ????? ??????? ?????? ? ???????? ????????????.
?????? ?????? ????????? ? ?????? – ??? ??????????? ?????????? ??????? ???????? ?? ????? ?? ???????????? ?????? ??? ?????? ????? ? ?????? ???????. ? ?????? ?????? ???????? ????????? ??????????? ????????? ???????????? ??????????, ????????????? ???????? ? ???????? ? ????????..
?????? ?????? ????????? – ??? ??????? ?????? ??????? ?????? ?? ??????????? ?? ???????????? ?????? ???????? ???????? ?????????? ? ?????? ???????. ? ?????? ?????? ??????? ????????? ????? ???????????? ???????? ??????????, ??????????????? ??????? ? ???????? ? ?????????..
?????? ??????? ?????? ???????? ????????????? – ??? ?????????? ? ??????????? ??????? ???????? ?????? ?????? ???????? ?????????????? ??????????. ????????? ??????????? ??????? ?????? ?? ???????????? ? ?????????? ???????????? ?????? ??????? ????????? – https://www.russkiy-diploms-srednee.com/. ???????????? ???????????? ? ?????? ?????? ???????, ??????? ????????? ? ?????? ? ??????? ?????, ?????????, ????????????? ????????? ? ????????. ??????? ??????????? – ??????????? ?????????? ?????? ????????? ????????, ????????????? ??????????? ? ??????? ????????. ??? ???????????? ?????????? ?????? ??? ???????? ? ???? ??????????? ??????????????? ?????? ??? ????????? ?????. ????? ?????, ??????? ????????????? ? ?????? ???????? ?????? ??????????? ? ??????????? ???????? ??? ?????, ??? ?????? ??????? ?????? ? ???????.
? ?????? ???????? ?????? – ??? ?????????? ? ???????? ?????? ????????? ?????? ???????? ???????? ?????????? ???????. ???????????? ??????????? ?????????? ??????? ?? ???????????? ? ?????????? ???????? ?????? ??????????????? ?????????? – http://www.orik-diploms-srednee.com. ??????????? ???????? ? ?????? ???????, ??????? ???????????? ? ????????????? ? ??????? ??????? ???????????, ?????????, ??????? ????????? ? ?????????????. ???????? ??????????? – ??????????? ?????????? ???????? ???????, ????????????? ??????????? ? ????????. ??? ???????????? ?????? ?????? ??? ????????????? ? ???? ??????????? ??????????????? ?????? ??? ????????????? ????. ????? ???????, ????? ????????????? ? ?????? ?????? ???????? ?????? ??????????? ? ??????????? ????????? ??? ???, ??? ?????? ??????? ?????? ? ????? ??????.
?????? ?????? ? ?????? ??????? ??????????? – ??? ??????????? ?????????? ???????? ?????? ?? ????????????? ??????? ?? ???????? ?????? ???? ???????? ????? ? ?????? ???????. ? ??????? ?????? ???????? ?????? ????? ????????? ???????????? ??????????, ??????????????? ???????? ? ???????? ? ????????..
???????? ?????? ????????????? ????? ?????? ?? ???????? ????.
?????? ????????????? ?????? ? ?????? ?????? ????????????? ?????? .
???????? ? ?????? ?????? – ??? ???????! ????????? ? ??????
????????? https://obivka-divana.ru/ .
?????? ?????? ? ?????? – ????? ?????? ???????? ??????????? ????????????? ? ?????????? ???????????????? ??????????. ?????? ????????? ???? ? ????? ????????? ???????????? ? ????????????????? ?????.
?????? ????!
???? ?? ? ??? ??????, ????? ??????????? ?????? ????????? ?????? ? ?????? ???????????? ?????? ??? ????????????? ??????? ??????? ??????????????? ? ????????????, ?? ????? ?? ????????? ? ?????????? ??????? ??????????? ? ??????? ????????, ??? ?.
??? ???, ??? ????? ?????????? ???????? ? ???????????? ?????????? ? ????, ??? ????????????? ???????? ? ???????? ???????????? ? ????????? ????????? ??????. ?????? ?? ????? ??????? ????? ?? ????????? ????????? ??? ??????????? ?????? ? ??????? ?????????????. ?????, ?? ???? ???????, ????????????? ???????? ?????? ??? ?????? ? ????????? ????????? ? ???????? ????? ? ????????? ???????? ? ????????? ?? ???? ??????. ?????? ???????????? ? ????????????? ??? https://1server-diploms.com, ??? ??????????? ????????!
?????? ?????? ?????? ???????
?????? ?????? ????????
????? ???? ?????????? ??????!
Gana premios con el bono casino sin deposito
bono de casino sin deposito casino online con bono sin deposito .
??? ??????? ?????? ???????? ????? ??? ??????? ?????? ???????
???????? ????? ?????? ? ?????????? ??????? ???? https://rulonnyygazon177.ru/ .
?????? ????????????? ? ???????? ???? – ????? ??????? ???????? ??????????? ????????????? ? ????????? ???????????????? ??????????. ?????? ?????????? ????? ? ????? ????????? ???????????? ? ?????????? ????????.
1. ????? ???????? ????? – ?? ????????? ???????
2. ???-5 ?????????? ???????? ???????? ?????
3. ?? ???????? ??????? ???????? ??????
4. ??????? ??? ??????? ?????: ????? ?? ??????
5. ?? ????????? ?????? ???????? ????? ?? ?????’????
6. ??????????? ?????????? ? ??????????? ???????? ?????
7. ??????? ????? ? ??????????? – ??????????? ??????? ??? ?????
8. ??????? ??????? ??????? ???????? ?????
9. ?? ?????????? ?? ???????????? ???????? ??????
10. ????? ??? ???????? ?????: ??? ????????
11. ???????? ??????? ??? ???????? ????? – ???????????? ?????
12. ?????? ?????????? ??? ???????? ?????: ?? ????????
13. ???? ?? ??????: ?? ?????????? ?????????? ??????? ?????
14. ??????? ????? ? ?????? ???????: ??????? ?? ????????????
15. ?? ???????????? ????? ? ?????????? ?? ????????? ???????? ?????
16. ????? ???????? ????? ? ????? ???????: ????????? ??????
17. ??????? ????? ?? ??????????? ????????? – ????? ????????? ???????
18. ???????????????? ? ??????? ?????????? ?????’???: ??????? ????? ? ??????
19. ?? ?????? ?????????? ??? ???????? ?????: ?????? ???????
20. ?????????? ??????? ???????? ?????: ??? ??????? ?? ???????????
????? ??????? ???? https://natjazhnistelitvhyn.kiev.ua/ .
??? ???????? ??? ????? ??????
4. ??????????? ??? ?? ????? 9?12: ?????? ? ???????
??????????? ??? ?? ????? 9?12 https://domizbrusa9x12spb.ru/ .
????????
13. ????? ?????????? ?????????? ??? ???????
??????? ??????????? ????? ???????? ??????? ?????????? ????? .
1. ?????? ????? – ??? ???????????? ??????? ??????
2. ??? ??????? ????????? ????? ??? ???????? ??????????
3. ?????? ??????: ??????? ????? ??? ?????????
4. 5 ???????? ?????? ????? ? ???????
5. ????? ????? ??????? ??? ????????????? ???????
6. ????? ?? ?????????: ??????? ? ????? ? ?????
7. ????? ????? ????? ????????? ? ???? ?????
8. ????-??? ??????: ??????? ????? ? ????? ????????
9. 10 ????????? ????????? ?????? ? ????????
10. ?????? ?????: ??? ??????? ?????? ??? ????????? ??????
11. ?????????? ????? ?? ???????: ????????? ??????? ??? ?????
12. ??????? ????? ?? ???????: ??? ????????? ?????????????? ????
13. ? ????? ????? ?????? ?????: ?????? ?? ?????????
14. ??? ????????? ????? ??? ????? ?????
15. ????? ?? ????????: ???????? ?????? ? ??????
16. ?????-?????: ????????????? ?????? ??? ?????? ?????
17. ? ??? ?????? ????? ?? ??????? ????????
18. ????? ? ?????????: ?????? ?? ???????
19. ??? ??????? ????? ??? ???????? ?? ???????
20. ???-5 ??????? ??????: ???????? ? ????? ? ?????
?????? ????? ??? ????? talan .
?????? ??????????
2. ?????? BMW – ?????? ????? ??? ?????????????
bmw x1 2023 bmw m2 2023 .
?????? ??????????? ?????? ????? ??????????? .
????????? ???????????
2. ??????? ??????? ????????????: ??? ?? ????? ??????????
3. ?????????????? ???????????: ???????? ???? ? ?? ????????????
4. ??? ?????????? ??? ??????? ????????????: ?????? ???????
5. ??????? ??????? ????????? ????????????: ?????? ?? ??????????????
6. ?????????? ???? ????????????? ???????????? ? ?????????
7. ???, ??? ??? ????? ????? ? ????????????: ???????? ??????????
8. ???????????: ????? ?????????? ??????? ? ?? ??????????????
9. ????? ? ?????? ????????????: ??? ????????? ??????? ????????
10. ??? ??????? ?????? ????? ? ??????? ????????????: ??????? ? ??????
11. ?????????????? ???????: ???? ? ?????????? ???????
12. ????????????? ????????????: ???? ??? ??????????? ???????
13. ??????????? ? ??????? ?????????: ??????????? ?????? ? ???????
14. ???????????? ???????????? ????? ??????? ????????????? ???????????
15. ??? ??????? ?????????? ?????????? ??? ?????? ? ?????????????
16. ???????????: ???????? ???????? ??? ???????????? ????
17. ??????????? ??? ??????? ??????: ????????? ??????? ??????????
18. ?????????? ??????? ????????????: ?????? ???????????? ??????
19. ??????? ? ???????? ????????????: ???????? ? ??????????
20. ????????????? ? ?????????????? ????????????: ???????? ????? ? ????????????
???????????? ????????? ?????? ?????? ???? .
?????????‚?? ???????»???? ?????µ???????°???°?‚?µ?»?? – ????? ??????? ??????? ??????????? ???????? ?? ????????? ???????????????? ??????????. ????????????? ????????? ???? ? ??????????? ????????? ???????????? ? ?????????? ????????.
https://server-attestats.com/ – ?????? ???????? ? ??????? ???????????- ????? ?????? ??????? ??????????? ???????? ? ????????? ???????????????? ??????????. ????????????? ?????????? ???? ? ????? ????????? ???????????? ? ?????????? ????????.
??????? ?????? ?????? ??????? ??????????? ??????? .
?????????!
??????? ? ?????? ?????? ???? ?????? ????????, ??????????? ? ? ???????????? ???????? ??????!
?????? ???????? ?? 11 ?????
??????????????? ?????
7. ?? ???????? ????? ????? ?????
???????????? ????? ?????????? ???? https://stomatologiyatrn.ivano-frankivsk.ua/ .
http://forum.ainsinet.fr/viewtopic.php?id=3&p=7 – ?”?????»?????‹ ?????????‚?? ?? ???‹???€?µ?? ???±???°?·?????°?????? – ??? ??????? ??????? ??????????? ????????????? ?? ????????? ???????????????? ??????????. ????????????? ?????????? ???? ? ??????????? ????????? ???????????? ? ?????????? ????????.
1. ???? ??? ??????? ?????????
2. ?????? ? ???????
3. ??? ??????? ????????? ???????? ?????? ? ???????
4. ??????? ????????? ??????-???????
5. ?????? ?????? ?????????
6. ?????? ???????
7. ?????? ??? ????????? ????????
8. ????????? ??????
9. ?????? ???????
10. ??????-??????: ??????? ????????? ??????? ? ????? ???????
11. ?????????? ????? ? ???????? ??????? ? XXI ????
12. ?????????? ???? ??? ??????? ?????: ???????? ???????????? ????? ?????
13. ????????? ? ????? ??????? ??????: ????????????? ????
14. ??????-????? ?? ???????? ????????? ??????? ????????
15. ????????? ???????????: ???????? ???????????? ??????? ? ????? ????
16. ?????? ????: ???????? ?????????? ??????? ? ?????? ?????????
17. ????????????? ???? ? ?????????????? ????????: ?????? ? ????
18. ???????? ????????? ??????? ? ???????: ??? ??????? ??????????? ????????????
19. ????? ?? ???????
20. ?????? ???????????? ???????
????????? ??????? ????????? ??????? .
split ??????? https://split-sistema-kupit.ru/ .
?????? ??????? ??? ????????? ????????????: ??? ??????
?????? ???????????? ???? ?????? ???????????? ???? .
http://???????.??/students/educational-resources/ – – ??? ?????? ??????? ??????????? ?????? ?? ?????????? ???????????????? ??????????. ?????? ????????? ???? ? ??????????? ????????? ???????????? ? ?????????? ????????.
???????? ??????
2. ??? ?? ?????: ????????? ???????????? ?????? ??????
3. ?????? ??????? ??? ????????? ???????????? ? ????????
4. ??????????? ??? ??????????????? ????????? ?????????????
5. 10 ????? ? ????????? ????????? ????????????
6. ????????? ?????????? ?? ????????? ???????????? ?? ???????
7. ?????? ?????? ????????? ???????????? ?? ?????
8. ??? ??????? ????? ??? ????????? ???????????? ? ???????
9. ??????? ???????? ????????? ???????????? ? ??????? ????
10. ????????????, ??? ????????? ?????????? ?????-???????
11. ??????????? ??????????? ??? ????????? ????????????
12. ????? ????????? ????? ??? ?????????? ????????? ?????????????
13. ???-5 ?????? ??? ??????????????? ????????? ????????????
14. ????????? ???????????? ?? ???????: ??????????? ? ??????
15. ????? ????? ????? ????????????? ??????????? ? ?????
16. ?????? ????? ???????? ????????? ???????????? ??????????????
17. ??? ????????????? ? ????????? ???????????? ? ?????? ?????
18. ????? ?? ????????? ?? ????????? ?????????????
19. ?????? ??????????? ???????? ???????????? ????? ??????????
20. ????? ?????? ???? ?????????????: ????????? ????? ??????????
???????????? ?????????? ? ????????????????? ???????????? ?????????? ? ????????????????? .
??????? ???? ???!
??????????? ?????????? ?????? ? ????????? ???????? ? ????????? ? ????? ????? ?????? ??? ??????????????? ?????? – ????????? ? ???????!
?????? ???????? ????????
? ??? ?? ?????? ???????? ????????? ?? ??????????? ???? ????? ?????? ? ????????? ?? ?? ? ???????????? ?????? ????? ?????????!
???????? ?????? ???? ? ????????? ?? ?????? ??? ?????????? ? ? ????????? ??????????? – ?????? ? ?????????!
?????????? ??????????? ? ???????? https://multisplit-sistemy-kondicionirovaniya.ru/ .
?????????!
?????? ?? ? ??? ??????, ????? ??????????? ?????? ????????? ?????? ? ?????? ?????? ?????? ??? ????????????? ??????? ??????? ??????????????? ? ???????????? ?????, ?? ????? ?? ??????? ? ?????????? ??????? ??????????? ? ??????? ????????, ??? ? ? ?????.
??? ???, ??? ????? ?????????? ???????? ? ???????????? ?????????? ? ?????????, ??? ????? ??????????? ????????? ??????? ???????????? ? ????????? ????????? ??????. ?????? ?? ????? ??????? ????? ?? ????????? ????????? ??? ??????????? ?????? ? ??????? ?????????????. ?????, ?? ???? ???????, ????????????? ???????? ?????? ??? ?????? ? ????????? ????????? ? ???????? ????? ? ????????? ???????? ? ????????? ?? ???? ??????. ?????? ???????????? ? ????????????? ?? , ??? ?????????!
https://komfort.rusff.me/post.php?fid=13
?????? ?????? ????
?????? ?????? ? ??????? ???????????
?????? ??????
?????? ?????? ????????
?????? ?????? ?????? ???????
????? ?????? ?????? ??????!
?? ????????? ???????? ???????? ??? ?????????? ???????
???????? ????? ???????? ???????? ????? ???????? .
?????? ???? ????!
?? ?????-?????? ?????? ?????? ? ?????? ?????? ??? ????? ???????????? ? ??????, ?? ????? ?? ????????? ? ?????? ??????? ????????, ??? ? ? ?????????)
??? ??? ????? ??????????? ? ??????? ??????????, ??? ????????????? ???????? ?? ???? ???????????? ? ????????? ???????, ?? ????? ??????? ????? ?? ?????????? ??? ??????? ? ????????? ?????????????, ??? ????? ???? ??????? ?????? ??? ?????? ? ????????? ???????? ? ???????? ? ????????? ? ????????? ?? ??????, ?????? ?????????? ????? , ?????????!
https://sun-clinic.co.il/he/question/%d0%ba%d1%83%d0%bf%d0%b8%d1%82%d1%8c-%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc-%d0%b2%d1%83%d0%b7%d0%b0-%d0%bf%d0%be%d0%ba%d1%83%d0%bf%d0%ba%d0%b0-%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc%d0%b0-%d0%b2-%d0%bc/
?????? ?????? ?????????
?????? ?????? ????????
?????? ?????? ?????? ???????
?????? ?????? ????
?????? ??????
????? ?????? ???????? ???????!
????????????!
?? ?????-?????? ?????? ?????? ? ?????? ?????? ??? ????? ???????????? ? ??????, ?? ????? ?? ????????? ? ?????? ??????? ????????, ??? ? ? ?????????)
??? ??? ????? ??????????? ? ??????? ??????????, ??? ????????????? ???????? ?? ???? ???????????? ? ????????? ???????, ?? ????? ??????? ????? ?? ?????????? ??? ??????? ? ????????? ?????????????, ??? ????? ???? ??????? ?????? ??? ?????? ? ????????? ???????? ? ???????? ? ????????? ? ????????? ?? ??????, ?????? ?????????? ????? , ?????????!
https://www.astrolabetech.com/topic/%d0%ba%d1%83%d0%bf%d0%b8%d1%82%d1%8c-%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc-%d0%b3%d0%be%d0%b7%d0%bd%d0%b0%d0%ba-%d0%bf%d0%be%d0%b2%d1%81%d0%b5%d0%b4%d0%bd%d0%b5%d0%b2%d0%bd%d1%8b%d0%b5/
?????? ?????? ??????
?????? ?????? ? ?????? ???????????
?????? ?????? ????
?????? ?????? ????
??? ?????? ??????
????? ??????? ?????? ???????!
??????? ???? ???!
?????? ?? ? ??? ?????, ??? ??????????? ?????? ????????? ?????? ? ?????? ?????? ?????? ??? ????????????? ??????? ???????? ??????????????? ? ??????????? ??????, ?? ????? ?? ???????? ???? ? ?????????? ??????? ?????????? ???????? ??????????, ??? ?.
??? ???, ??? ????? ?????? ???????? ? ????????????? ?????????? ? ????, ??? ????????????? ???????? ? ???????? ???????????? ? ????????? ????????? ??????. ?????? ?? ????? ??????? ????? ?? ????????? ????????? ??? ?????????? ??????? ? ????????? ?????????????. ?????, ?? ???? ???????, ????????????? ???????? ?????? ??? ?????? ? ????????? ????????? ? ???????? ????? ? ????????? ???????? ? ????????? ?? ???? ??????. ?????? ???????????? ? ????????????? ?? ????? , ??? ?????????!
https://sontopic.com/blogs/1374/«???????-?????????-?-??????-???????????
?????? ?????? ???????????
?????? ?????? ?????????
?????? ?????? ? ??????? ???????????
?????? ?????? ? ?????? ???????????
?????? ?????? ????
????? ???? ???????? ???????!
Los mejores juegos de casino en linea en Peru
mejor casino online peru mejor casino online peru .
????????????!
???? ?? ? ??? ?????-?????? ???, ??? ??????????? ?????? ????????? ?????? ? ????? ?????? ?????? ??? ????????????? ??????? ???????? ??????????????? ? ????? ???? ????? ??????, ?? ????? ?? ???????? ???? ? ?????????? ??????? ?????????? ???????? ??????????, ??? ?.
??? ???, ??? ????? ?????? ???????? ? ???????????? ?????????? ? ?????????, ??? ????????????? ????????? ??????? ???????????? ? ????????? ????????? ??????. ?????? ?? ????? ??????? ????? ?? ????????? ????????? ??? ?????????? ??????? ? ??????? ?????????????. ?????, ?? ???? ???????, ????????????? ???????? ?????? ??? ?????? ? ????????? ????????? ? ???????? ????? ? ????????? ???????? ? ????????? ?? ???? ??????. ?????? ???????????? ? ????????????? ?? ????? , ??? ?????????!
http://little-witch.ru/forum99.html
?????? ?????? ?????????
?????? ?????? ?????? ???????
?????? ?????? ? ??????? ???????????
?????? ?????? ????????
?????? ?????? ? ??????
????? ?????? ?????? ???????!
??????? ????????
– ???? ??? ????????? ?????????: ????????? ? ???????
????? ??????? ??????????? ????? ??????? ??????????? .
??????, ??????? ????????!
?????? ?? ? ??? ?????, ??? ??????????? ?????? ????????? ?????? ? ?????? ?????? ?????? ??? ????????????? ??????? ???????? ??????????????? ? ??????????? ??????, ?? ????? ?? ???????? ???? ? ?????????? ??????? ?????????? ???????? ??????????, ??? ?.
??? ???, ??? ????? ?????? ???????? ? ????????????? ?????????? ? ????, ??? ????????????? ???????? ? ???????? ???????????? ? ????????? ????????? ??????. ?????? ?? ????? ??????? ????? ?? ????????? ????????? ??? ?????????? ??????? ? ????????? ?????????????. ?????, ?? ???? ???????, ????????????? ???????? ?????? ??? ?????? ? ????????? ????????? ? ???????? ????? ? ????????? ???????? ? ????????? ?? ???? ??????. ?????? ???????????? ? ????????????? ?? ????? , ??? ?????????!
https://antiozuevo.0bb.ru/viewtopic.php?id=4923#p24326
?????? ?????? ????
?????? ?????? ?????????
?????? ?????? ??????
?????? ?????? ? ?????? ???????????
?????? ????????
????? ??????? ?????? ???????!
?????????!
???? ?? ? ??? ??????, ????? ??????????? ?????? ????????? ?????? ? ?????? ???????????? ?????? ??? ????????????? ??????? ??????? ??????????????? ? ????????????, ?? ????? ?? ????????? ? ?????????? ??????? ??????????? ? ??????? ????????, ??? ?.
??? ???, ??? ????? ?????????? ???????? ? ???????????? ?????????? ? ????, ??? ????????????? ???????? ? ???????? ???????????? ? ????????? ????????? ??????. ?????? ?? ????? ??????? ????? ?? ????????? ????????? ??? ??????????? ?????? ? ??????? ?????????????. ?????, ?? ???? ???????, ????????????? ???????? ?????? ??? ?????? ? ????????? ????????? ? ???????? ????? ? ????????? ???????? ? ????????? ?? ???? ??????. ?????? ???????????? ? ????????????? ??? , ??? ??????????? ????????!
http://ekonomimvmeste.ukrbb.net/viewtopic.php?f=8&t=24624
?????? ?????? ? ?????? ???????????
?????? ?????? ? ??????? ???????????
?????? ?????? ?????????
??? ?????? ??????
?????? ?????? ????????????
????? ?????? ?????? ??????!
??????, ??????? ????????!
?????? ?? ? ??? ?????, ??? ??????????? ?????? ????????? ?????? ? ????? ???????????? ?????? ??? ????????????? ??????? ??????? ??????????????? ? ???????? ?????, ?? ????? ?? ????????? ? ?????????? ??????? ?????????? ???????? ??????????, ??? ??, ??? ? ?.
??? ???, ??? ????? ?????????? ???????????? ???????? ??? ?????? ? ??????? ??????????, ??? ????????????? ????????? ??????? ???????????? ? ????????? ????????? ??????. ?? ????? ??????? ????? ?? ????????? ????????? ??? ??????????? ?????? ? ????????? ?????????????. ????? ???????????? ???????? ?????? ??? ?????? ? ????????? ????????? ? ???????? ????? ? ????????? ???????? ? ????????? ?? ???? ??????. ?????? ???????????? ? ????????????? ?? ?????? , ??? ??????????? ??????!
https://eiron.myblog.arts.ac.uk/forums/topic/%d0%ba%d1%83%d0%bf%d0%b8%d1%82%d1%8c-%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc-%d0%be-%d1%81%d1%80%d0%b5%d0%b4%d0%bd%d0%b5%d0%bc-%d0%be%d0%b1%d1%80%d0%b0%d0%b7%d0%be%d0%b2%d0%b0%d0%bd%d0%b8%d0%b8/
?????? ?????? ? ?????? ???????????
??? ?????? ??????
?????? ?????? ?????????
?????? ???????? ?????
?????? ?????? ????????
????? ??????? ?????? ??????!
??????, ??????? ????????!
?????? ?? ? ??? ?????, ??? ??????????? ?????? ????????? ?????? ? ?????? ?????? ?????? ??? ????????????? ??????? ???????? ??????????????? ? ??????????? ??????, ?? ????? ?? ???????? ???? ? ?????????? ??????? ?????????? ???????? ??????????, ??? ?.
??? ???, ??? ????? ?????? ???????? ? ????????????? ?????????? ? ????, ??? ????????????? ???????? ? ???????? ???????????? ? ????????? ????????? ??????. ?????? ?? ????? ??????? ????? ?? ????????? ????????? ??? ?????????? ??????? ? ????????? ?????????????. ?????, ?? ???? ???????, ????????????? ???????? ?????? ??? ?????? ? ????????? ????????? ? ???????? ????? ? ????????? ???????? ? ????????? ?? ???? ??????. ?????? ???????????? ? ????????????? ?? ????? , ??? ?????????!
https://satitmattayom.nrru.ac.th/?dwqa-question=%d0%ba%d1%83%d0%bf%d0%b8%d1%82%d1%8c-%d0%b4%d0%b8%d0%bf%d0%bb%d0%be%d0%bc-%d0%ba%d0%be%d0%bb%d0%bb%d0%b5%d0%b4%d0%b6%d0%b0-%d0%b6%d0%b8%d0%b7%d0%bd%d0%b5%d0%bd%d0%bd%d1%8b%d0%b5-%d1%81%d0%bb%d1%83
?????? ?????? ? ??????
?????? ?????? ?????????
?????? ?????? ????
?????? ?????? ????????
?????? ????????
????? ??????? ?????? ??????!
https://man-attestats24.com – ?????? ???????? ?? 11 ????? – ???? ??? ?????? ????????????. ?? ????? ??????? ??? ?? ??????? ????? ? ?????? ?????? ????????, ?????? ??? ???????????? ???????? ??? ???????????????. ???? ??????????? ???????????? ??????? ???????? ? ??????????? ?????????????? ?????. ??????????? ??????????????? ???????? ? ????? ??????? ? ???????? ?????? ??????????? ??? ????, ????? ?????? ????????????????? ????? ? ???????.
??????, ??????? ????????!
?????? ?????? ????
????? ??????? ????????????? ???????!
http://www.livecenter.ru/index.php?showtopic=737&mode=linear
?????? ?????? ????
??? ?????? ??????
?????? ??????
?? ?????? ????????? ????????? ??????
??????? ?? ?????????
?????? ???????? ??????? https://ryukzakivijskovibpjgl.kiev.ua/ .
??? ????????? ??????? ??????????
???? ???????????? ??????? .
?????? ???? ????!
?????? ?????? ??????
????? ?????? ??????????) ???????!
http://artem-energo.ru/forums.php?m=posts&q=16669&n=last
?????? ?????? ? ?????? ???????????
?????? ?????? ???????????
?????? ?????? ? ??????? ???????????
Hello are using WordPress for your site platform? I’m new to the blog world but I’m trying to get started and create my own. Do you require any coding expertise to make your own blog? Any help would be really appreciated!
#be#jk3#jk#jk#JK##
?????? ????????? ??????
https://arusak-attestats.ru – ?????? ???????? ? ?????? – ??????????? ??? ?????? ????????????. ? ?????? ??????? ??? ?? ??????? ??? ????? ? ?????? ???????? ????????, ?????? ??? ??????????? ????????? ??????????? ??? ????????????????? ?????. ???? ???????? ???????????? ???????? ? ??????????? ?????????????? ?????. ????????? ??????????????? ???????? ????? ? ???????? ????? ??????????? ??? ?????? ?????????? ???????? ? ???????????????.
?????????!
?????? ?????? ? ??????? ???????????
????? ?????? ?????????? ???????!
https://artem-energo.ru/forums.php?m=posts&q=16669&n=last
??? ?????? ??????
?????? ?????? ?????????
?????? ?????? ????????????
? ????? ????????, ??? ???????? ???????? ??????? ???????? ??????? ? ????? ???????????, ?????? ???? ??????????? ??????? ? ??????? ???? ????????? ????????????? ???????????. ???? ??????? ????????? ?? ??????????? ?????? ???????????. ???? ?????? ????????? ????? ????? ?????? ?????????, ??????? ?????????? ?????? ???????? ???????????? ??? ??????? ? ?????-???? ?????????.
???? ???????? ?????????? ??????????? ?????? ???????? ???? ??????????? ????????. ?? ??????? ?????????? ????????, ? ??? ?????????? ???????? ???????? ??? ????????, ??????? ?? ???? ????????? ??????????? ??? ??????? ????????. ????? ???????? ??????????????? ?????????, ? ?????? ????????? ? ?????????? ???????. ?? ?????? ?? ???????? ????????? ???????????? ????????.
???????????? ????? ??????? ??????? ?? ?????? ? ???, ??? ????? ?????????? ???????? ???? ????????. ???? ??????? ??????????? ?????? ? ?????, ? ????? ??????????. ?? ?????? ??????????? ??????? ????????? ?? ??????????? ?????????? ?????? ?????? ? ???????? ? ????? ????? ?????? — ??? ??? ?????????? ????????? ????? ????????.
????, ??? ???? ??????????? ??????? ?????? ???????? ????????? ????????, ???? ???????? ?????????? ???????? ???????. ?????? ???????? – ??? ?????? ???????? ??????????? ???????? ? ????? ?????????? ? ????? ?????: ? ??????????? ? ??? ??? ? ?????? ???????? ???????.
http://prema-attestats.ru/ – ????? ?????? ????????
?????????!
?????? ?????? ????????
????? ???? ?????? ??????!
http://mail.u-turn.kz/forums.php?m=posts&q=23921
?????? ?????? ? ??????? ???????????
?????? ??????
??? ?????? ??????
????????????!
?????? ?????? ????
????? ??????? ???????? ???????!
http://borderforum.ru/topic8527.html
?????? ?????? ????
?????? ?????? ? ??????? ???????????
?????? ?????? ????????????
Hmm is anyone else experiencing problems with the images on this blog loading? I’m trying to figure out if its a problem on my end or if it’s the blog. Any suggestions would be greatly appreciated.
#be#jk3#jk#jk#JK##
????? ???????? ??????????
pharmacy website india http://indiaph24.store/# ?»?legitimate online pharmacies india
online shopping pharmacy india
pharmacies in mexico that ship to usa: Online Pharmacies in Mexico – mexican pharmaceuticals online