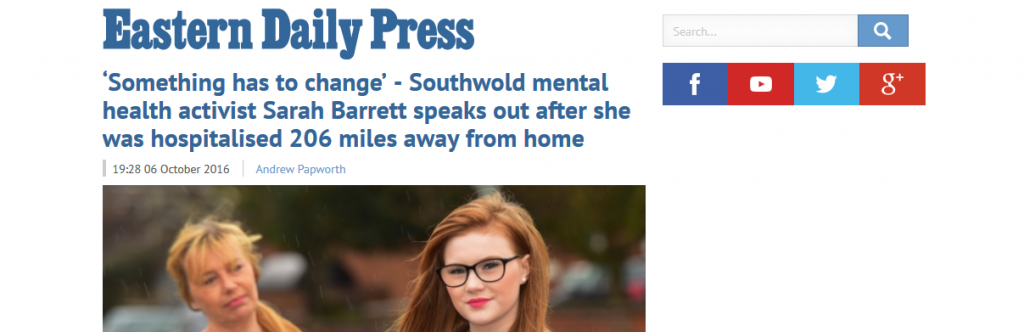
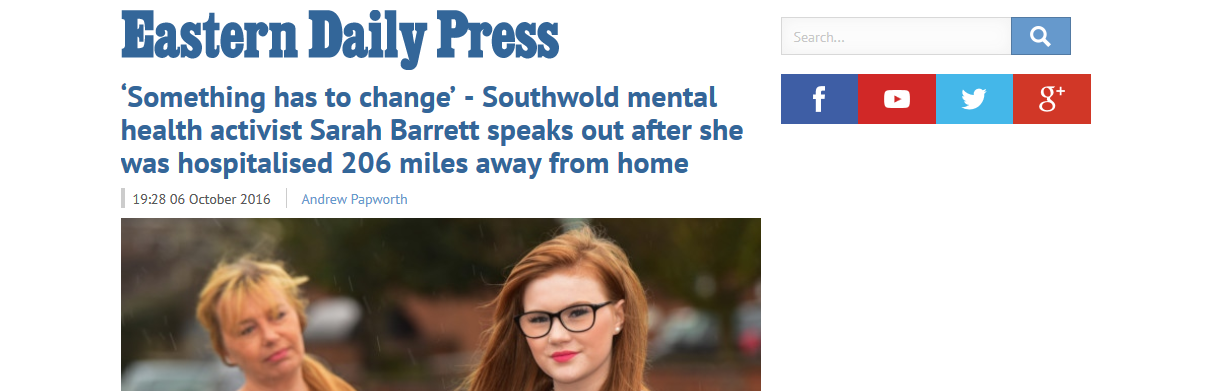
No wonder the Eastern Daily Press has been shortlisted for a mental health journalism award. Andrew Papworth reports:
A teenage mental health patient sent to hospital 206 miles away from home while recovering from post-traumatic stress disorder (PTSD) after a violent assault has said: “We must campaign for local hospitals.”
Sarah Barrett was 16 and studying for her GCSEs when, at her own request, she was admitted to a mental health unit following several suicide attempts. But with a shortage of beds closer to home, the closest available hospital was in Southampton – 206 miles from her home near Southwold.
That, she said, made her recovery even harder in what was already a horribly difficult situation.
Alison Armstrong, director of operations (Suffolk) at Norfolk and Suffolk Foundation Trust – which runs mental health services in the area – said it could not comment on individual cases.
Of course she can, with the permission of the patient and the family who have already chosen to speak to the press. Armstrong often claims this but it is untrue.
Armstrong continues:
“We fully understand the distress out of area placements can cause service users and their families particularly at a time when they are at their most vulnerable. We aim to have no patients being treated out of area and we are working with commissioning colleagues to develop innovative solutions for services we are currently not commissioned to deliver.
“If this is not possible as all of our beds are full, we will always seek a bed within area with other providers or in a neighbouring county, such as Cambridgeshire or Essex, before looking further afield.”
Beds have been full for at least the last three years. NSFT closed Waveney Acute Services at Carlton Court, the hostel beds and beds at the Fermoy Unit in King’s Lynn even though they were needed. NSFT wanted to close all the acute beds in King’s Lynn until we forced a partial u-turn. NSFT closed beds for older people and now the dire situation is about to become worse as 24 more beds are closed at the Julian Hospital.
The Care Quality Commission (CQC) told NSFT eighteen months ago that NSFT needed to ensure it had enough local beds for local people and NSFT promised its regulator, Monitor, that it would deliver sufficient beds. NSFT and commissioners have done little about the beds crisis despite the Norfolk CCGs having promised in January 2014 to end out of area placements by May 2014. NSFT is still blowing its budget on private beds. The beds crisis is as bad as ever and in fact becoming worse as there are sometimes no NHS or private hospital beds available anywhere in the country. The lack of NHS beds is costing lives: we have a deaths crisis.
Sarah said: “Something has to change. We must recognise that sending people who are ill miles from their families and friends makes it much, much harder for them to recover and also causes additional problems. We must campaign for local hospitals because I wouldn’t wish what happened to me to happen to anyone else.”
Sarah added:
“I was already extremely homesick and I couldn’t just pick up the phone and call my mum to come and see me – she couldn’t afford to drive 206 miles.
“There was no funding for her – she was stuck in an awful situation where there was nothing she could do but listen to me scream and cry down the phone that I wanted to come home.
“I wasn’t able to focus on my recovery for weeks.”
Her mother Cath Pickles said: “It was costing about £300 every time I went to see here and I very quickly went through the money I had. It’s just immoral.”
Thank you to Sarah for bravely speaking out.
Join us at the NSFT AGM on Thursday 20th October to demand decent funding for mental health and an end to the deaths whitewash.
Read the story and support investigative journalism by buying the EDP. You can also read the story on the EDP website by clicking on the image below: