Norfolk and Suffolk NHS Foundation Trust (NSFT) sent dishonest letters to hundreds of children and young people on waiting lists.
NSFT claims that the dishonest discharge letters were a ‘mistake’ but refused to answer the BBC’s reasonable questions about what happened and what it is doing about put things right. We don’t even know what the ‘mistake’ was. We suspect the ‘mistake’ was getting found out.
What has been going on?
At the end of February 2020, the CQC inspected the Youth Service of mental health services for Children, Families and Young People (CFYP) at NSFT.
It was disastrous. Not just for waiting lists but it is waiting lists on which we will focus below.
CQC found:
We were not assured that processes for managing waiting lists, particularly team-held waiting lists, kept people safe. Where a patients’ risk was discussed in team meetings and there was an identified change to risk, we saw that risk assessments were not always updated. There was no clear process to ensure patients on team-held waiting lists were appropriately monitored and supported. We saw large gaps in records, with one patient not having had direct contact since July 2019. Patient waiting list concerns had been mentioned at the last four inspections and it was disappointing that this had not been fully addressed within this team.
So, CQC had expressed concerns at the last FOUR inspections.
There was no clear process to ensure patients on teamheld waiting lists were appropriately monitored and supported. We saw gaps in records; one patient had not been contacted since July 2019. Another patient had several attendances at the acute hospital emergency department whilst waiting for allocation, the GP had followed up with concerns and in the summer of 2019 the liaison staff at the Accident and Emergency department submitted an incident report due to the lack of availability for support from the youth team. A further patient had been referred to the team in March 2019. The patient was added to the waiting list for a care co-ordinator in July 2019 but only made it to the priority meeting in January 2020. We were not assured that processes for managing waiting lists, particularly team-held waiting lists, kept people safe.
This mismanagement has serious, perhaps fatal, consequences:
We reviewed the early learning report from a recent serious incident. We saw that at the time of the incident, the patient had recently been seen by clinicians. However, in the months prior to this we saw missed opportunities to engage with the patient, cancelled appointments and cancelled group sessions due to staff sickness. We saw evidence of a decline in the patients mental health that was not immediately acted upon. The patient was on the teamheld list and did not have one single clinician overseeing their care. This is currently subject to a full root cause analysis investigation that has not yet been completed.
Front line NSFT staff told CQC that there were not the resources to provide a service to those on waiting lists:
The staff member was concerned that the team was expected to address the waiting list for assessment without the resource in place to then offer support identified in this process.
We believe the despicable and dishonest decision to discharge hundreds of children and young people, rather than provide the resources and competent management to deliver promised care to them, was made by the leadership of the CFYP Care Group and the operational management of NSFT, probably with knowledge and approval of the executive Board. It also appears likely that the local representatives of CQC were aware of what NSFT was doing.
NSFT’s latest Board papers let us see what was happening to waiting lists in CFYP around the time of the CQC inspection in February 2020:
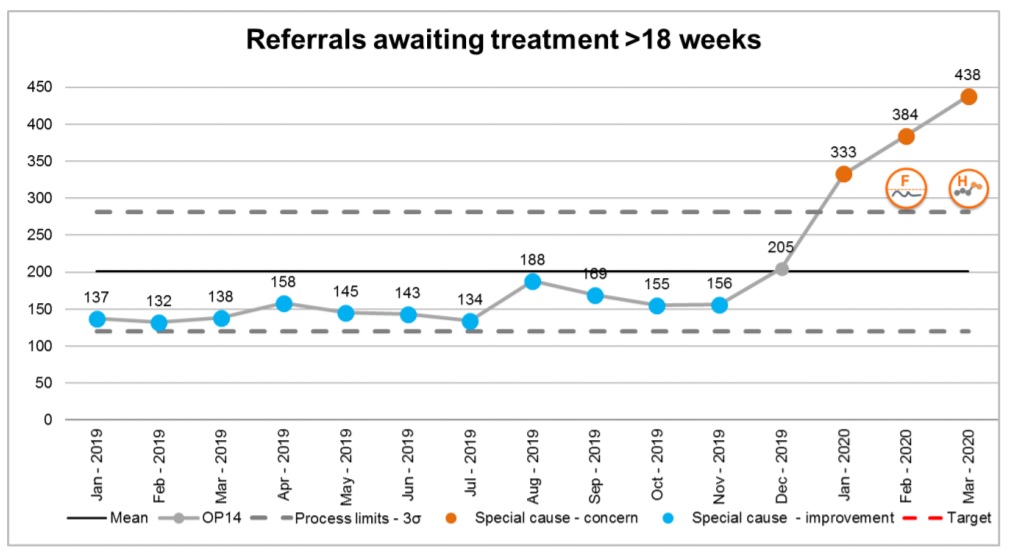
The ‘Integrated Performance Report’ states:
225 (51.4%) relate to CFYP services in Norfolk and Waveney, up 19 from 206 in February 2020… the system will be expected to consistently fail this target and that performance is now reporting as a cause for concern in special cause variation.
So, more than half of all breaches of the 18 weeks waiting time limit were due to CFYP in Norfolk and Waveney. Even before the CQC inspection, NSFT’s Board knew the serious problems were endemic in CFYP.
The February 2020 CQC inspection report tells us:
In response to the concerns raised within this report, the trust leadership team provided assurance of action which had begun just prior to the inspection. For instance, on 13 February 2020, an executive-led rapid improvement board had been established. This aimed to accelerate improvements and have senior leadership oversight.
NSFT’s ‘trust leadership team’ and an ‘executive-led rapid improvement board’ with ‘senior leadership oversight’ must have known of and approved the plan to discharge hundreds of children and young people from waiting lists.
The CQC inspection report also tells us that:
The care group leadership team were spending 4 to 5 days per week at St Stephens Road. We were told of plans to undertake a large-scale clinical review of the waiting list early in March 2020.
It seems impossible that the care group leadership team could have been unaware of the decision to abuse the Covid-19 epidemic to dishonestly discharge hundreds of children and young people from waiting lists for treatment, given they were spending four to five days per week at 80 St Stephen’s and told the CQC of their plans ‘to undertake a large-scale clinical review of the waiting list’. Indeed, the ‘Advice and Signposting Team’ which was supposed to help discharge the children and young people without promised treatment is widely acknowledged to be the ‘baby’ of the CFYP Service Director, Rob Mack. We’ve already said that Rob Mack should be sacked.
The care group leadership reported to Amy Eagle, the disgraceful appointment as £90k+ Deputy Chief Operating Officer of NSFT, who has an appalling track record of closing and cutting services at 80 St Stephen’s. Eagle reports to Stuart Richardson, the £120k+ Chief Operating Officer of NSFT, who has created chaos in his nearly two years at NSFT. It seems inconceivable that Eagle and Richardson did not know what was going on at 80 St Stephen’s. If they knew, they were complicit; if they didn’t know they were incompetent. Both have outstayed their welcome at NSFT. In fact, neither should have been employed in the first place.
It appears that even NHS Improvement has lost patience with Eagle, Richardson and the NSFT Board. We were told that there would no longer be an Improvement Director when Marie Gabriel and former Professor Warren were installed as Chair and Chief Executive as NSFT ‘no longer needed one’. However, the May 2020 Board papers tell us:
An Improvement Director has been appointed with NHSI to support the trust and will focus initially on CFYP.
The new ‘Director of Improvement’, James Innes, a pharmacist, has just completed a health leadership masters and looks far below the calibre of previous Improvement Director, Alan Yates. But he wouldn’t have to do much to be an improvement on Yates’ successor as Improvement Director, Philippa Slinger. But will he have the skills, experience and authority to challenge the appalling and inept but devious and self-serving management clique at NSFT?
What did the rest of the NSFT Board know?
What were the Chief Nurse, Diane Hull, and Chief Medical Officer, Dan Dalton, doing while all this was going on?
What did CQC know?
Is this what ‘improvement’ looks like?
How much longer can children and young people be made to pay the price of the NSFT Board’s incompetence?
There is more to tell and many more questions for NSFT to answer.
Stay tuned.