Geraldine Scott, Health Correspondent of the Eastern Daily Press, reports:
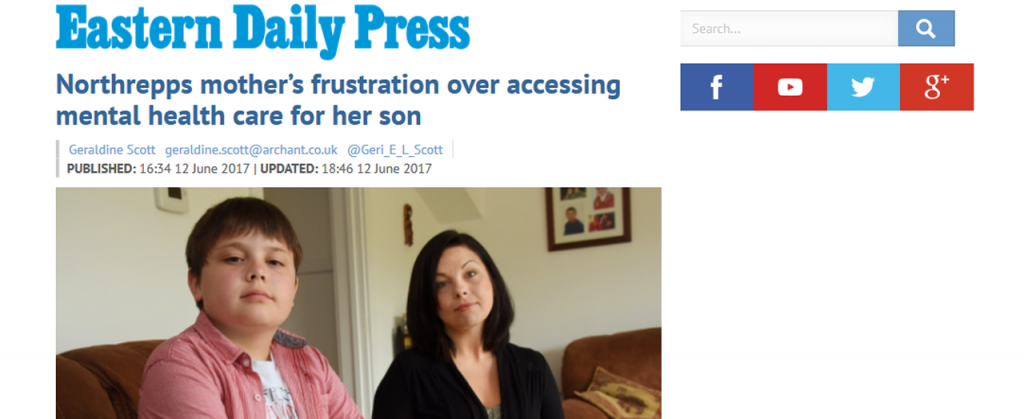
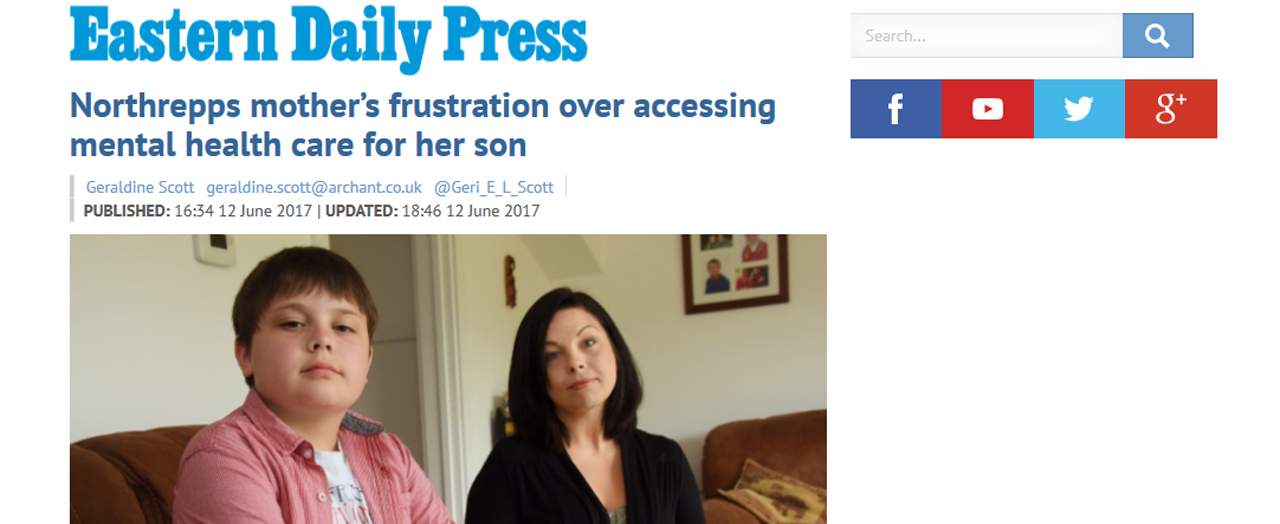
Michelle Kimp, 35, has struggled to get the appropriate medical treatment for her 12-year-old son Robert – who has aspergers and ADD – for around seven years.
Mrs Kimp said due to his conditions Robert had depression and had spoken about taking his own life.
But she said after bounced being between children and young people’s mental health services – known as CAHMS – and his paediatrician, she was told last November that “suicide is not necessarily mental health”.
“It was an incredibly long process to get a diagnosis in the first place,” said Mrs Kimp, who lives in Northrepps.
“The first time we went to CAHMS Robert had not been diagnosed at this point and they said he did not have a mental health problem.
“I said ‘he’s trying to kill himself, tell me that if I end up finding him dead’.”
Mrs Kimp is far from the first parent to be forced to say this to the Children, Family and Young Person (CFYP) Service.
Services for young people in Suffolk provided by Norfolk and Suffolk NHS Foundation Trust (NSFT) have already been condemned by a joint Ofsted/CQC inspection.
Mrs Kimp said she was particularly conscious of the risk as her cousin took his own life aged 16.
“It’s as if he’s got to seriously harm himself, harm someone else or kill himself before someone will help him,” she said.
No wonder the suicide rate in North Norfolk has increased by a staggering 77 per cent between 2010-12 and 2013-15.
Mrs Kimp believes the issues with treatment come because children on the autistic spectrum do not tick the right boxes.
“I went to a post diagnosis meeting a few weeks ago and was told this was normal because there isn’t the funding for autistic children with mental health. Because they present differently to ‘normal’ children with mental health issues, no one will treat them. It’s disgusting.”
Now, she wants to highlight how difficult the fight is, to try and raise awareness of the problem.
A spokesman for Norfolk and Suffolk NHS Foundation Trust, the region’s mental health trust, said young people with conditions such as Robert’s would usually be treated by their multi-disciplinary Neuro-Developmental Disorders Team and could stay with that team up to the age of 26.
They added: “We take suicidal thoughts or behaviours expressed by children and young people very seriously.
Why then has the suicide rate in North Norfolk increased by more than TWELVE times the national average increase?
“Every young person coming into our trust’s Children, Families and Young People’s services receive a full, and holistic assessment of their mental health needs, taking into consideration their social situation, family history and school or work life.”
This isn’t what we hear. Mrs Kimp’s experience is far from atypical.
CAMHS services at NSFT experienced the deepest cuts in England.
While patients waited months to be seen, one of NSFT’s CFYP consultants, on a salary of more than £150,000 per year, who was a coincidentally a trust cheerleader for the radical redesign cuts and establishment of ‘Youth’, was swimming and enjoying long lunches at UEA during the working day. We and others have raised the issue of ‘medical productivity’ at private meetings, at public NSFT Board meetings and personally with the Chair of NSFT, Gary Page, but no urgent or effective action is taken.
The Chair of NSFT and its executives know they have a minority of doctors on six-figure salaries who are seeing less than half a dozen patients in clinic per week but they are too weak or unbothered to do anything about a patently disgraceful situation. It is a Faustian Pact: the doctors don’t mention the appalling mismanagement, the management don’t address the minority of lazy doctors. But patients and their families pay the price.
To be clear, most doctors at NSFT work extremely hard. But a significant minority do not.
How can NSFT offer safe or effective secondary mental health services if some of its doctors aren’t seeing the patients in their area in clinic?
Patients, carers and front line clinical staff care deeply about waiting lists and lack of treatment but NSFT’s Board doesn’t seem to care about anything other than eating biscuits and drinking tea. There is no genuine voice of the patient and carer at NSFT.
NHS Improvement tried to help us bring about change on this vital issue but NSFT has even resisted its own regulator. We’ve been forced to go to local MPs – they find the situation outrageous. Physical health hospitals or GP practices wouldn’t tolerate doctors seeing one patient per day and nor should mental health.
New Ways of Shirking has to stop. If Bohdan Solomka is too weak to address this issue, NSFT needs a new external appointment to Medical Director.
Another consultant cheerleader for the disastrous radical redesign has a new job with the shiny-new perinatal service, now that Youth and EI services are under stress. When community mental health services were cut to shreds, the same cheerleader consultant left behind their slashed community mental health team and patients and took a new job with the shiny-new Youth Service. Despite £2.5m funding and an enormous salary bill for two consultants, the new perinatal service won’t start operating anything like fully until September. Time for more NSFT tea and biscuits. We hear from other areas of the country that their perinatal services have opened much more promptly. Don’t get ill if you’re pregnant, NSFT is in no rush.
Even more worryingly, we hear that NSFT has adopted its own definition of perinatal mental health which means that women with existing mental health conditions won’t be able to access the full service – just those who are ‘pure’ and have developed mental health problems for the first time during pregnancy. Women with existing mental health conditions who become pregnant have to stay in the generic and overwhelmed community mental health teams, apparently.
If true, we’d say that’s shocking discrimination.
Click on the image below to read the story in full on the EDP website: